Frozen Shoulder/Adhesive Capsulitis
Frozen shoulder or Adhesive Capsulitis is a shoulder condition in which the shoulder becomes painful with a progressive loss in range of motion and movement over time. Often this occurs without any specific injury, although it can occur after an accident. Additionally, some medical conditions, like diabetes, are associated with an increased risk of frozen shoulder.
Frozen Shoulder Causes.
Frozen shoulder can be divided into two groups. The first group is called the “idiopathic group.” Idiopathic means that the frozen shoulder occurred without any specific cause. The second group is called the “post traumatic group.” Post-traumatic frozen shoulder happens as a result of an injury, such as a broken arm. Most patients fall into the idiopathic group, i.e. the group who has frozen shoulder without any specific cause. There is a small group of patients who have frozen shoulder that is associated with a certain medical conditions, such as diabetes. It is unknown why diabetes places people at a higher risk for frozen shoulder.
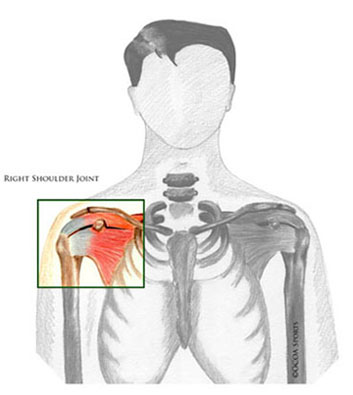
The shoulder is a ball and socket joint. A soft tissue layer called a capsule, similar to a balloon, surrounds the joint.
Frozen shoulder is also called “adhesive capsulitis.” Patients who have frozen shoulder develop irritation of the surrounding soft tissue capsule layer. This inflammation is called capsulitis. Frozen shoulder is called adhesive capsulitis because the inflamed capsule causes the shoulder to become tight or adhesed or stuck. Over time, the capsulitis inflammation resolves, but the stiffness remains. Eventually the stiffness resolves as well.
Most patients who have frozen shoulder are women between the ages of 35 and 65. Patients who have frozen shoulder on one side have a 20% chance of developing a frozen shoulder on the other. In addition, frozen shoulder that is associated with a medical condition, such as diabetes, carries with it a 40% chance of getting frozen shoulder on the opposite side.
Phases of frozen shoulder.
Frozen shoulder syndrome can be divided into three phases: freezing, frozen, and thawing. During the freezing phase, patients notice aching pain, often without any specific injury preceding the pain. They will complain of pain at night and they complain of pain at the endpoints of all their ranges of motion. Motion in this stage, however, is usually normal or slightly decreased. Though, when patients attempt to move their arm beyond their endpoint of range of motion, they experience significant pain. The freezing stage occurs when the capsulitis is developing and the shoulder is quite inflamed.
The next phase is the frozen phase. During this phase, the pain is typically significantly improved; however, motion is drastically reduced. Because of the significant motion loss, patients typically have difficulty doing day-to-day activities such as dressing, driving, or washing in the shower. Additionally, patients typically have a very hard time sleeping on the specific shoulder that is frozen. The frozen stage corresponds to improvement in the inflamed capsulitis.
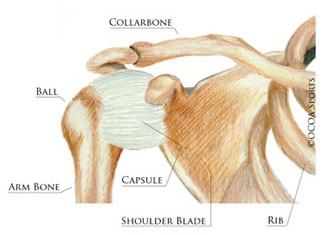
The capsule surrounds the joint
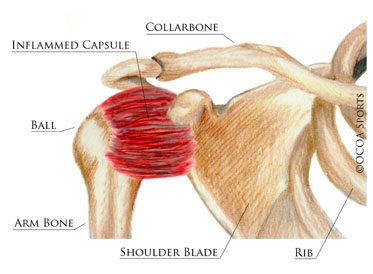
The capsule becomes inflamed and stiff
The final phase is called the thawing phase. During this phase, the frozen shoulder resolves. There is a steady improvement in motion and comfort over several months. Usually full motion and strength are regained, however, sometimes there is some element of motion loss and patients are instead left with near normal strength and motion.
Frozen shoulder can last up to 18 months, even with treatment. Patient’s typically progress through the three stages of frozen shoulder, freezing, frozen, and thawing. Eventually the inflammation, pain, and stiffness resolve.
Frozen Shoulder Treatment.
The mainstay of treatment for frozen shoulder is pain medication and physical therapy. Surgery is rarely required. Pain medication for frozen shoulder can be given in the form of pills or injections of cortisone or both. Sometimes, sleeping pills are also required because of the degree of discomfort from frozen shoulder. Surgery is rarely required and is reserved only for cases in which physical therapy has failed to effect any improvement in motion after several months. Otherwise, physical therapy is an important part of the treatment for frozen shoulder coupled with a home exercise program that is prescribed by the doctor and the therapist.
Frozen Shoulder Surgery.
Frozen shoulder rarely requires surgery. Most cases of frozen shoulder resolve over time. If your doctor recommends surgery, the procedure performed is a manipulation under anesthesia. ” This procedure allows the surgeon to move the shoulder, to improve motion, and break up scar tissue that has caused the shoulder to become stiff. During the procedure, the patient is asleep so that they do not feel any pain or remember the procedure. After the patient is asleep, the surgeon moves the shoulder through a full range of motion in a controlled fashion in order to break up any scar tissue and adhesions that have formed. Occasionally, shoulder arthroscopy is required in addition to the manipulation procedure in order to fully release any scar tissue.
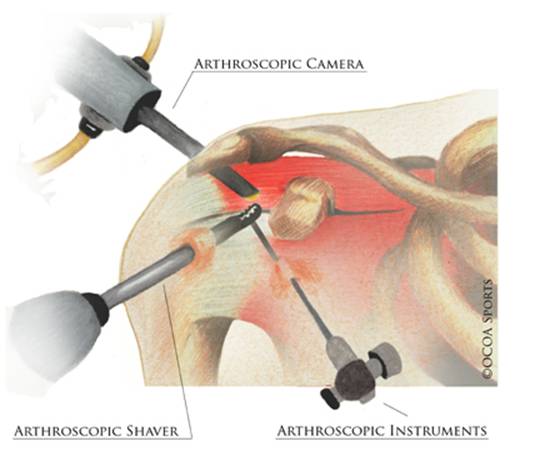
Arthroscopic camera and tools in the shoulder
Arthroscopic surgery uses small incisions and small tools, about the size of a pencil, to perform the procedure. All the work is visualized with a small camera, the arthroscope. The surgeon sees inside the shoulder with the arthroscope and its images are projected on a video screen.
Surgery for frozen shoulder does not cure the disease, it only improves motion. After the surgical procedure is performed, patients undergo intense physical therapy in order to maintain the motion that was achieved by the surgeon in the operating room. The pain from a frozen shoulder does not improve after surgery, only motion. Pain medication, however, is prescribed so that patients are comfortable after surgery and during therapy. Eventually, the pain from the procedure and inflammation resolve, and motion is restored.
If you’re suffering from orthopedic pain, whether or not it’s caused by a frozen shoulder, contact the doctors at Orlin & Cohen, the leading Long Island orthopedic practice. Immediate appointments are available: Schedule yours now.



